TFEB in stress adaptation, senescence, and aging
-
Cells rely on lysosomes and autophagy to maintain homeostasis under fluctuating environmental and metabolic conditions. However, how these degradative systems are dynamically coordinated across stress, senescence, and aging remains incompletely understood. ...
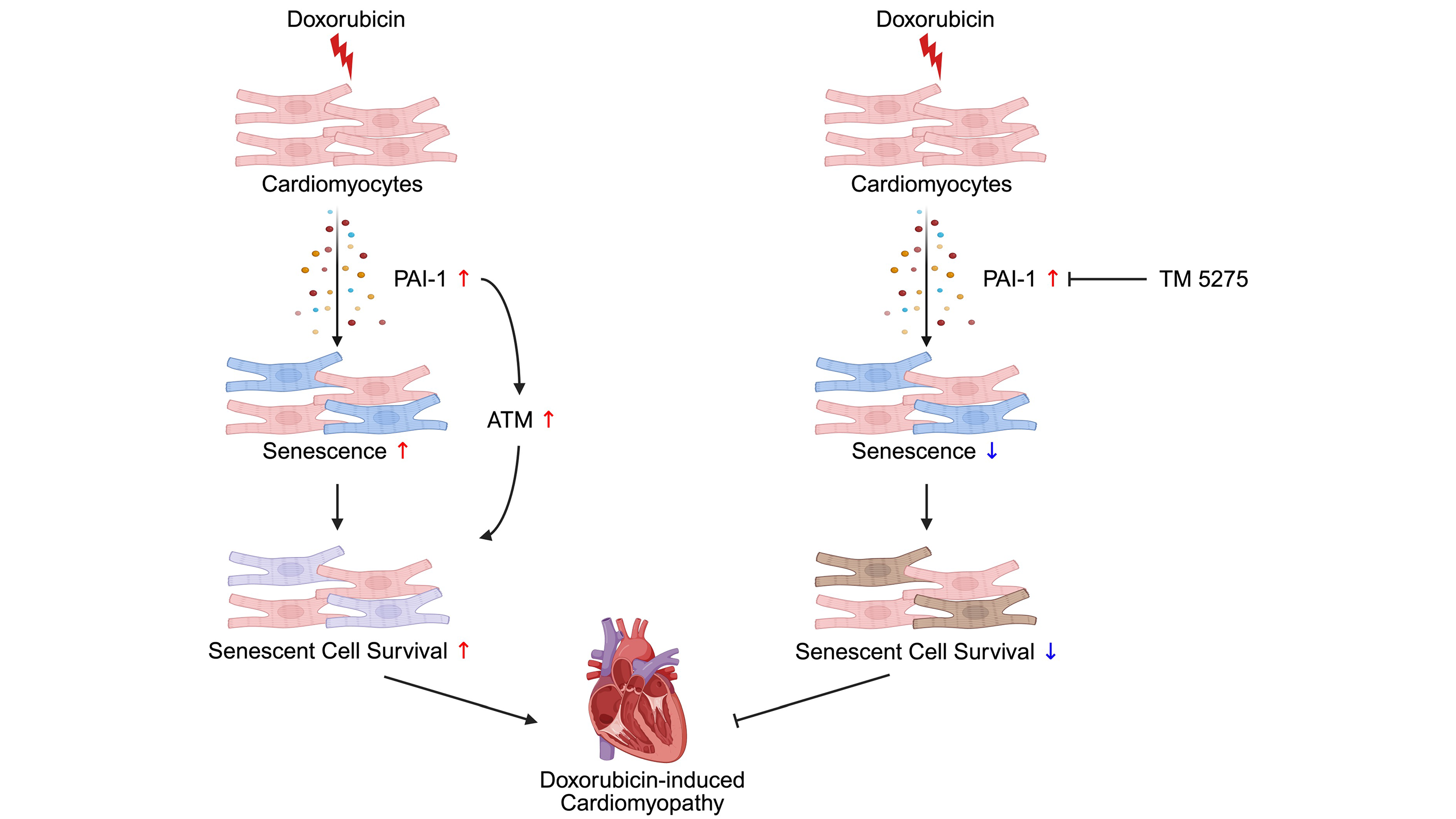
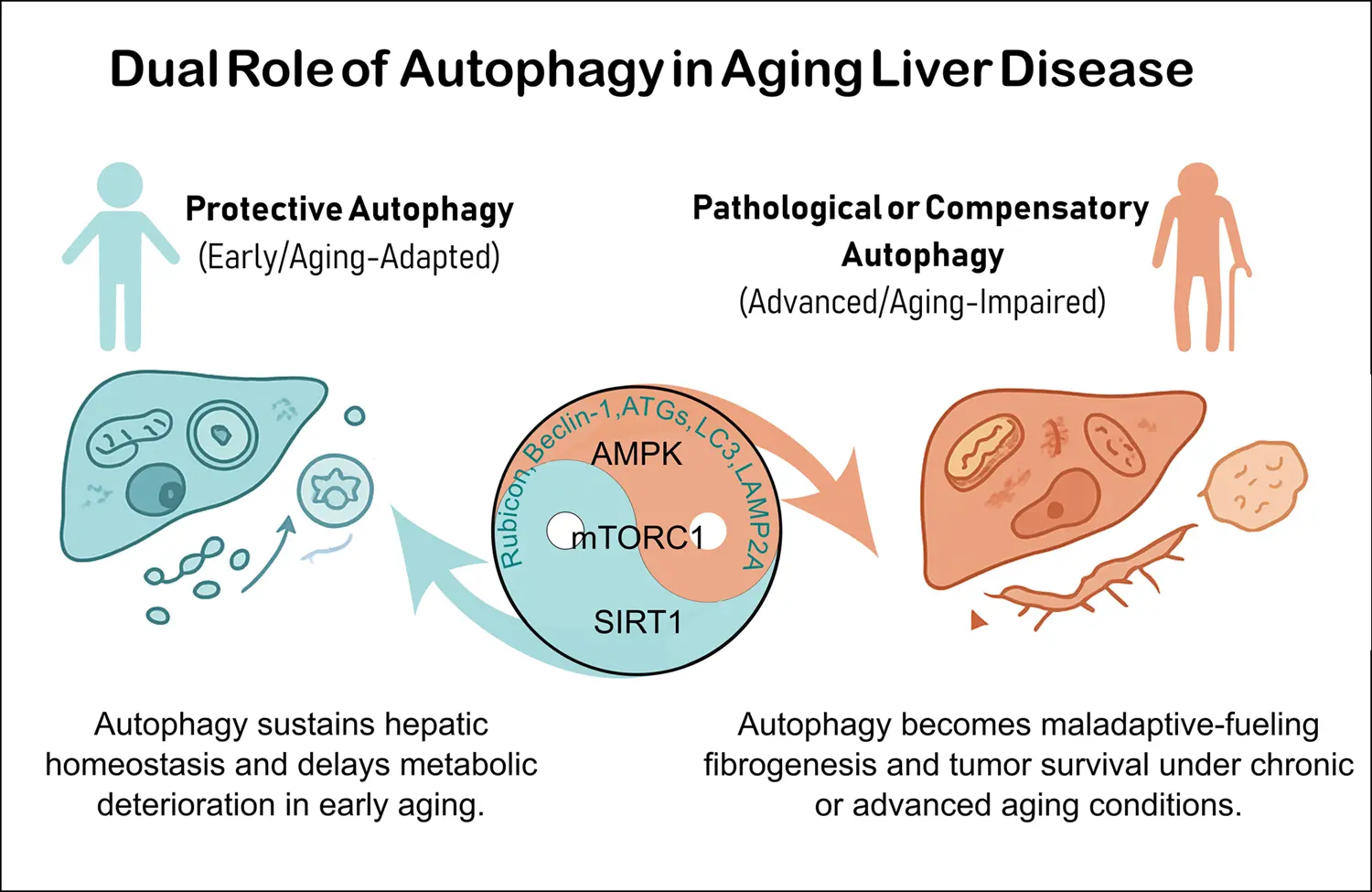
MoreCells rely on lysosomes and autophagy to maintain homeostasis under fluctuating environmental and metabolic conditions. However, how these degradative systems are dynamically coordinated across stress, senescence, and aging remains incompletely understood. Transcription factor EB (TFEB), a member of the microphthalmia/transcription factor E (MiT/TFE) family, has emerged as a key regulator of lysosomal biogenesis and autophagy by controlling the coordinated lysosomal expression and regulation (CLEAR) gene network, integrating nutrient sensing, mitochondrial status, Ca2+, redox signaling, and mechanistic target of rapamycin complex 1 (mTORC1) activity. While TFEB activation promotes lysosomal and metabolic adaptation during acute stress, accumulating evidence indicates that its activity is tightly constrained in time and magnitude, and that altered TFEB dynamics critically shape cellular fate decisions. Here, we synthesize current findings showing that transient TFEB activation supports stress resilience and recovery. In contrast, persistent, insufficient, or dysregulated TFEB signaling contributes to divergent senescence trajectories and age-associated decline in proteostasis. We further discuss how defects in TFEB regulation underlie impaired autophagy–lysosome function during aging across tissues. Notably, both insufficient and excessive TFEB activity can be maladaptive. Together, this framework positions TFEB as a dynamically regulated node linking stress adaptation, senescence progression, and aging, and highlights the need for context- and tissue-specific strategies aimed at restoring TFEB responsiveness rather than constitutively enhancing its activity.
Less -
Lena Guerrero-Navarro, ... Maria Cavinato
-
DOI: https://doi.org/10.70401/Geromedicine.2026.0024 - May 09, 2026